Until Covid-19 made its murderous debut in the U.S., the withering of the nation’s public health care system had gone largely unnoticed. The response to the epidemic has been so ineffectual as to call into question the U.S.’s status as a “developed” nation.
Progressive reformers who established the nation’s public health system at the turn of the 20th century understood that the effort was not only a humanitarian pursuit but a bulwark against the spread of disease that does not distinguish between rich and poor. Many New Deal administrators influenced by the Progressive movement held a holistic vision of public health. Hence, their stress on architecturally attractive hospitals often brightened by WPA artworks, as well as the New Deal’s vast expenditures on water treatment, nutritional classes, community clinics and child care. Today, that vision is as scarce as the PPE stockpile was when the coronavirus arrived on our shores.
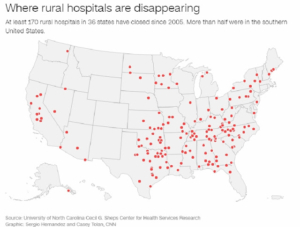
Two maps tell the story. One produced by the University of North Carolina shows at least 170 rural hospitals that have closed in the last 15 years, half of them in Southern states where the virus is now making rapid inroads. The other map displays the 822 hospitals built, repaired or improved between 1933 and 1939 by the Public Works Administration (PWA). When work by other New Deal agencies like the WPA, FERA and NYA is added, the national inventory of rural hospitals leapt to 5,304.
PWA Administrator Harold Ickes noted in 1939 that “There was, and there still is, a great need for small but modern general hospitals in rural areas all through the country,” while pointing to the hundreds of general hospitals built with PWA funds.
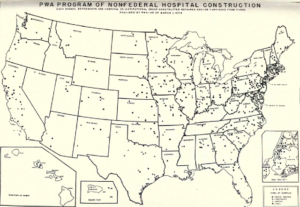
"America Builds: The Record of PWA”, 1939
New Deal work programs built and improved thousands of hospitals and clinics.
Photo Credit: Courtesy, National Archives
October 31, 2020, marked an important milestone in American public health: the 80th anniversary of the dedication of the campus of the National Institutes of Health (NIH), located in Bethesda, Maryland at which FDR spoke to the NIH’s role in the “conservation of life,” and using the power of science “to do infinitely more” for the health of all people with “no distinctions of race, of creed, or of color.”
Yet, today fully 25 percent of U.S. rural hospitals are at a high risk of closing, unless their financial situations improve, says an analysis by consulting firm, Guidehouse. It reports that rural hospitals and their communities are facing a crisis that has been lingering for decades.

Movable TB isolation unit, 1937
WPA-built huts, delivered to the patient’s own backyard, protected the family from infection.
Photo Credit: Courtesy, National Archives
Data published recently in The Guardian reveals the cost that tax cuts and the Great Recession have taken on the U.S.’s pandemic preparedness. “There are 2.9 hospital beds for every 1,000 people in the United States. That’s fewer than Turkmenistan (7.4 beds per 1,000), Mongolia (7.0), Argentina (5.0) and Libya (3.7). This lack of hospital beds is forcing doctors across the country to ration care under Covid-19, pushing up the number of preventable deaths.”
During the New Deal, legions of jobless were trained and hired to administer to the sick, prevent illness, both physical and mental, and construct public health infrastructure from hospitals and clinics to parks and playgrounds. As author and activist Naomi Klein explains, the New Deal’s investment in public health extended to delivering portable “isolation huts” for those afflicted with tuberculosis, enabling their families to safely and affordably care for them. The backyard huts were built by young men working for the National Youth Administration. State Boards of Health, which arranged regular visits by health workers, distributed the huts. Unlike testing for Covid, these lifeline services were federally funded, widely available and offered free of charge.

Mobile clinic
The Farm Security Administration brought health care to agricultural workers.
Photo Credit: Klamath County, Oregon. Photo courtesy LOC
Health was a very personal issue for Franklin Roosevelt after polio paralyzed him in 1921. Among the economic rights to which he insisted all Americans are entitled was “The right to adequate medical care and the opportunity to achieve and enjoy good health.” Unwelcome as it is, the current pandemic provides us with insight into a public health system we should have built upon but instead forgot we ever had.
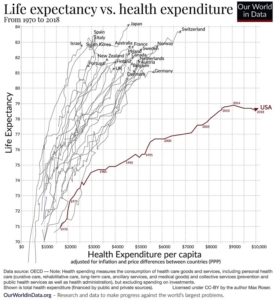
Life expectancy vs. health expenditure
Americans pay more for healthcare per capita and live shorter lives than do citizens in any other advanced economy
Photo Credit: Ourworlddata.org. With thanks to: richardbrenneman.wordpress.com

Water treatment plant, Michigan City, Indiana
PWA projects brought clean water to millions of households.
Photo Credit: Courtesy, National Archives, 1933-1943